What Relieves Interstitial Cystitis?
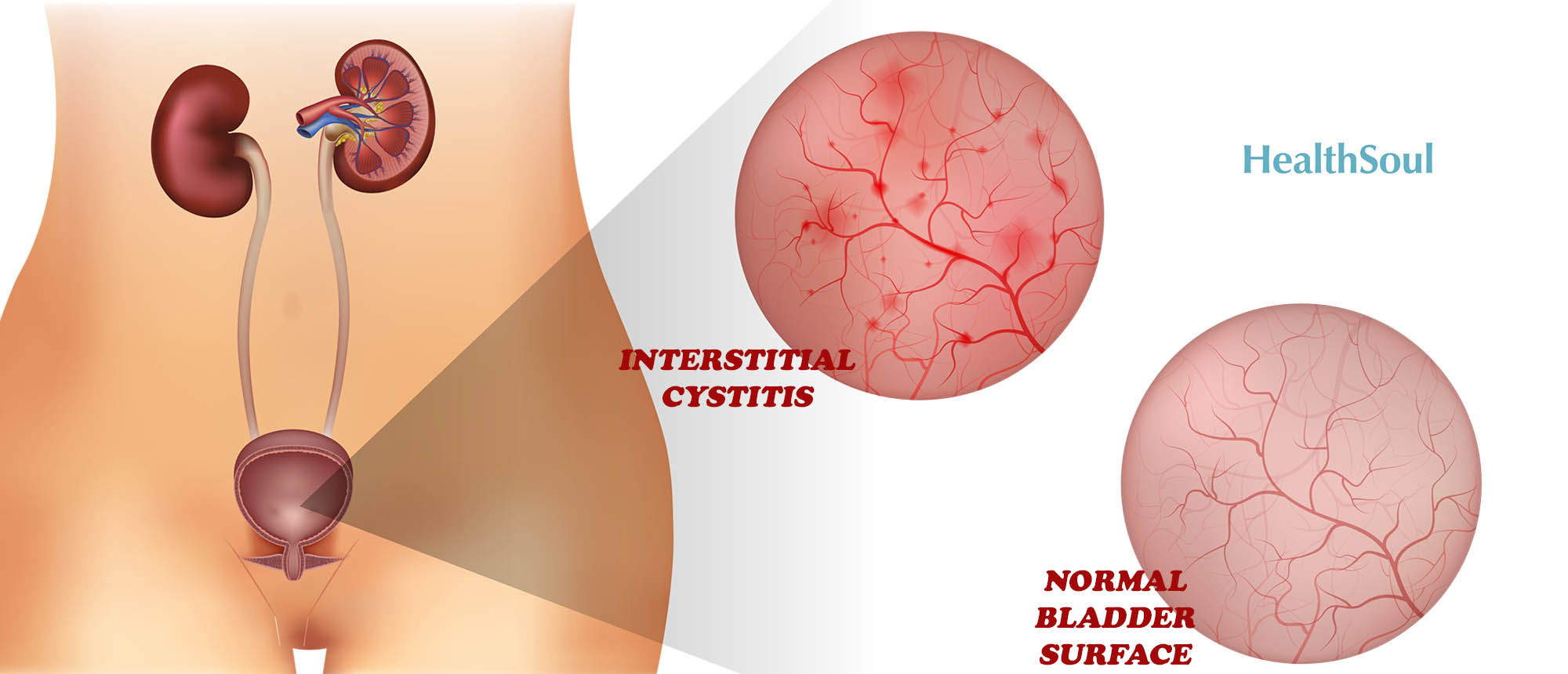
What Relieves Interstitial Cystitis?
Between the urgent need to run to the bathroom to chronic fatigue syndrome arising from sleeplessness due to nighttime urination, a diagnosis of IC can be devastating. Although there is no known cure for IC, many IC patients have seen a significant improvement in their symptoms by learning more about the root cause of IC and making lifestyle changes to manage symptom control.
What is Interstitial Cystitis (IC)?
The Interstitial Cystitis Association defines interstitial cystitis (IC) as a chronic condition of the bladder that involves multiple symptoms. Many IC patients experience recurring pelvic pain and pressure, discomfort in the bladder and pelvic region, and urinary frequency and urgency. IC is also commonly referred to as painful bladder syndrome (PBS), bladder pain syndrome (BPS), and chronic pelvic pain syndrome, and is often associated with other conditions such as endometriosis.

Symptoms of Interstitial Cystitis (IC)
The symptoms of interstitial cystitis vary from IC patient to IC patient. If you have IC, your symptoms may vary over time, including periodic flaring due to sexual activity, menstruation, sitting for a long time, stress, and exercise.
Common symptoms of IC include pain in the pelvis or between the vagina and anus in women or pain between the scrotum and anus in men, chronic pelvic pain, a chronic and urgent need to urinate due to an overactive bladder, pain during sexual intercourse, and bladder pain and discomfort while the bladder fills.
The severity of IC symptoms varies per individual. Some people experience pain-free sexual intercourse and symptom-free periods, while others experience mild discomfort. For many IC patients, the symptoms of IC may seem like similar symptoms to a urinary tract infection (UTI).
The severity of symptoms can worsen with sexual activity, antidepressants, allergies, certain medications, urinary tract infections, and menstrual cycles. About one-third of individuals with IC also have irritable bowel syndrome.

Diagnosis
If you’re experiencing persistent bladder pain and urinary urgency, contact your doctor. According to the American Urological Association, the basic diagnostic criteria of IC include a careful history, physical examination, and laboratory examination to assess symptoms of IC/BPS. Because the diagnosis of IC is often a diagnosis of exclusion, your doctor may need to perform additional procedures to rule out a bladder infection, endometriosis, ulcers, and other confusable conditions.
Your doctor will consider your medical history and may ask you to keep a bladder diary to record the volume of fluids you drink and urine you pass throughout the day. Additionally, your doctor may perform a physical exam to examine your pelvic area, vagina, and cervix and to assess your internal pelvic organs. To rule out urinary tract infection, your doctor will perform a urine culture.
A cystoscopy can also help your doctor confirm your diagnosis of IC. Your doctor will insert a thin time with a small camera (cystoscope) into the urethra to examine your bladder lining. To measure your bladder capacity, your doctor may perform a hydrodistention procedure in which he or she injects liquid into the bladder. Doctors typically perform this procedure after IC patients have been numbed with an anesthetic medication.
During your cystoscopy (while you’re under anesthesia), your doctor may perform a biopsy of the urethra and bladder to check for signs of bladder cancer and rarer conditions that cause bladder pain.
Your doctor may also perform a potassium sensitivity test. During a potassium sensitivity test, your doctor will perform place two solutions (water and potassium chloride) into the bladder and ask you to rate the urinary urgency you feel after each solution. When patients notice a significant variation in urgency or discomfort with the potassium solution, doctors may give a diagnosis of IC. Individuals with normal bladders cannot tell the difference between the two solutions and do not provide a significant variation in response.

Causes of Interstitial Cystitis (IC)
According to the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK), the exact cause of painful bladder syndrome/interstitial cystitis is unknown. However, many factors contribute to PBS/IC. IC patients have a defect in the protective lining of the bladder, which may allow toxic substances in urine to irritate the bladder wall.
Risk Factors
Multiple risk factors are associated with an increased risk of interstitial cystitis. IC has a higher prevalence in women compared to men. While symptoms in male IC patients may resemble interstitial cystitis, they’re more often due to inflammation of the prostate gland (prostatitis).
Skin and hair color can also contribute to an increased risk of interstitial cystitis. IC has a higher prevalence among individuals with fair skin and red hair. IC patients are most often diagnosed during their 30s or older.

Finding Relief
Interstitial cystitis can negatively affect your quality of life. Although support from friends and family is important, some IC patients may find the topic difficult to talk about. After your diagnosis of IC, the next step is to find a supportive doctor who is concerned about your quality of life. The right doctor will help you find the best way to relieve your urinary urgency, urinary frequency, chronic pain, and discomfort.
Many IC patients also benefit from joining a support group, seeking therapy, or participating in clinical trials for the treatment of interstitial cystitis. Ask your doctor for support group resources or visit the Interstitial Cystitis Association’s website for more information.
Many individuals with IC also find relief from making lifestyle changes. If you find that specific foods irritate your bladder, create a list of those foods and practice an elimination diet. For instance, if eating tomatoes causes symptom flares, eliminating tomatoes from your diet can relieve the discomfort of interstitial cystitis.
Physical therapy can help strengthen the pelvic floor muscles and reduce pain in the pelvic region. Bladder training with the help of a urologist (which involves timed urination), wearing loose clothing, and smoking cessation may also relieve painful bladder syndrome.

Treatment Options for Interstitial Cystitis Patients
No single treatment eliminates the symptoms of IC, and no single treatment works for every IC patient. IC patients may need to try combinations of different treatments before finding an approach that works.
Many doctors recommend working with a physical therapist to relieve pelvic pain stemming from muscle tenderness, muscle abnormalities, or restrictive connective tissue in the pelvic area.
Oral medications can also help IC patients manage symptom control. Common oral medications for IC include nonsteroidal anti-inflammatory drugs, including ibuprofen and naproxen sodium, to relieve pelvic pain and discomfort. Antidepressants—specifically tricyclic antidepressants, such as amitriptyline—can help IC patients relax their bladder and reduce pain. Antihistamines, like loratadine, can reduce urinary urgency and help relieve other IC symptoms.
In the United States, pentosan polysulfate sodium (Elmiron), another oral medication, has been approved by the Food and Drug Administration (FDA) specifically for the treatment of IC. Pentosan polysulfate sodium restores the inner surface of the bladder, protecting the bladder wall from potentially toxic substances in the urine. If you’re concerned about the side effects of oral medications, talk to your doctor.
Nerve stimulation, including transcutaneous electrical nerve stimulation (TENS), can relieve pelvic pain, reduce urinary frequency, and increase blood flow to the bladder. Some individuals with BPS/IC also notice a significant improvement in symptoms after cystoscopy with bladder distention, which involves stretching the bladder with water.
Bladder instillation, in which a doctor administers prescription medication dimethyl sulfoxide (DMSO) into your bladder through a catheter inserted through the urethra, can also help treat IC. Depending on the severity of your symptoms, the DMSO solution may be mixed with other medications, such as general anesthesia.
Finding the root cause of your BPS/IC symptoms often involves multiple procedures and treatment combinations. But for many individuals with IC, significant improvement and symptom control is possible.


