Vulvar cancer: overview, symptoms, causes, diagnosis and management
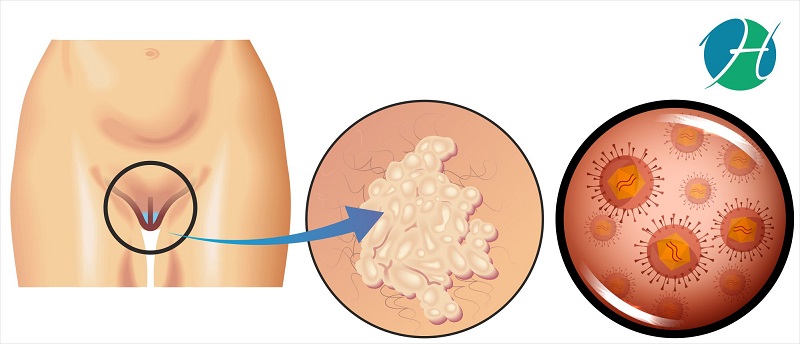
Vulva is the externally visible area of female genitalia. It is the area of skin that surrounds the urethra and vagina which is located between the upper thigs of women. Cancer affecting this region of the female body is known as vulvar cancer. Part of the vulva surrounding the vagina as two skin folds or lips is known as labia. Cancer of labia is the most common form of vulvar cancer. It can cause pain, itching or bleeding and affects the women’s ability to participate in sexual activities.
It usually affects women in the age group of 65 to 75 but it can occur at any age. It is the fourth most common gynecological malignancy in the United States. Vulvar cancer causes about 6000 new cases and 1000 deaths every year in United States.
Signs and symptoms
Symptoms depend upon whether the problem is cancerous or precancerous. Precancerous lesion may have no symptoms at all or rarely have persistent itching and thickened vulvar skin. Most of the patients suffering from vulvar cancer will experience symptoms which may include
- Vulvar itching that doesn’t go on its own
- Burning sensation
- A lump or painful nodule
- Thickening of vulvar skin
- Pain in the vulvar region
- Cut or ulceration in the skin
- Bleeding from the vulva which is different from menstruation

Causes
Cancer occurs when the genetic material of the cells gets mutated causing unstoppable division of cells. Other normal cells start starving and the cancerous cell proliferate forming nodules or tumorous growth. The exact cause of vulvar cancer is not known but there are some risk factors which increase the occurrence of mutation in the genetic material that includes
Increasing age: though vulvar cancer can occur at any age but it is seen that it is frequently diagnosed in females at an average age of 68
Exposure to human papilloma virus (HPV): HPV is a virus that is sexually transmitted. Many individuals acquire infection after getting exposed to this virus but this infection goes away on its own. Studies have shown that infection with HPV can increase the chances of mutation in the genetic material thus increasing the risk of several cancers like vulvar and cervical. Multiple sex partners, unsafe sexual practices and weaker immune system increase chances of acquiring HPV.
Smoking: smoking is associated with many cancers. One of the cancers is vulvar too.
Precancerous condition: some conditions like vulvar intraepithelial neoplasia or lichen sclerosus of vulva have tendency to give rise to cancer. If detected early, these conditions can be managed easily
Prior history of cervical cancer.

Diagnosis
Many of the above-mentioned symptoms can be caused by other noncancerous conditions also. Therefore, it is important to differentiate the other symptomatic benign disease from the vulvar cancer. Your doctor will ask you a detailed history of symptoms and possible risk factors you might have been exposed to. Physical examination and tests may will be required to certain the diagnosis
Physical examination: your doctor will examine the complete pelvis for the presence of any visible growth, ulceration or any other abnormalities. It can be done with the help of colposcope.
Biopsy: There are various benign condition that can mimic cancers and therefore It becomes difficult to certain whether the visible growth or any abnormality is cancerous or not. It is advised to take samples of the affected tissue, through the process known as biopsy and then inspecting the cells present in the tissue under the microscope. It will help to certain whether the lesion is cancerous or not. It will also help to determine the histological type of vulvar cancer. There are various histological types of vulvar cancer of which squamous cell carcinoma is the most common type comprising of at least 75 % or more of the total cases and melanoma is the second most common.
Once it is confirmed that an individual is suffering from cancer. It becomes important to assess the staging. Staging is determined to the extent a cancer has been spread. Staging the cancer helps to decide the best suitable management modalities to be used and determine the prognosis. Staging is usually done by the help of imaging tests such as magnetic resonance imaging (MRI) or PET-CT scan.

Management
Management of vulvar cancer will depend upon cancer type, staging and the health of the patient. There are usually three management options for cancerous growth, that are surgery, chemotherapy and radiotherapy. Most of the times combination of these are used to treat the cancer.

Surgery
For the cancers which are restricted to the vulvar region or haven’t been spread so far can be removed with the help of surgery. A small amount of normal tissue surrounding the cancerous lesion is also removed to reduce the chances of recurrence. For extensive cancers, entire vulva along with the affected structures may need to be removed surgically. Radiotherapy or chemotherapy may be used prior to surgery to shrink the size of tumor.
Radiation therapy
Radiation comprises of high energy beams that kills the cancer cells. It is delivered by an external device that delivers the radiation at precise points thus killing cells in that area. It can be used prior to surgery to shrink tumor size or after it to kill the left out cancerous cells.
Chemotherapy
Chemotherapy uses drugs which are toxic to growing cells. For advance staged cancer which have been spread to the different parts of the body chemotherapy is the usual option. Since, it affects the growing cells, normal cells of the body also get killed. So, chemotherapy has side effects too.
Prognosis
Women in the United States have 0.3 % lifetime risk of being diagnosed with vulvar cancer. Cancer stage at the time of diagnosis has a strong influence on length of survival. Survival rates are used to compare the survival of cancer patients with survival of other people in general population who are of the same age, race and sex. The overall five-year survival rate of vulvar cancer after diagnosis was 71.1 % but advance staged cancers have much lower survival rates.
References
- Siegel RL, Miller KD, Jemal A. Cancer Statistics, 2017. CA Cancer J Clin 2017; 67:7.
- Schuurman MS, van den Einden LC, Massuger LF, et al. Trends in incidence and survival of Dutch women with vulvar squamous cell carcinoma. Eur J Cancer 2013; 49:3872.
- Madsen BS, Jensen HL, van den Brule AJ, et al. Risk factors for invasive squamous cell carcinoma of the vulva and vagina–population-based case-control study in Denmark. Int J Cancer 2008; 122:2827.
- Saraiya M, Watson M, Wu X, et al. Incidence of in situ and invasive vulvar cancer in the US, 1998-2003. Cancer 2008; 113:2865.
- Yamamoto R, Sakuragi N, Shirato H, et al. Radiotherapy with concurrent chemotherapy for vulvar adenocarcinoma associated with extramammary Paget’s disease. Gynecol Oncol 2001; 80:267.
- Sugiyama VE, Chan JK, Shin JY, et al. Vulvar melanoma: a multivariable analysis of 644 patients. Obstet Gynecol 2007; 110:296.
- https://www.cdc.gov/cancer/vagvulv/basic_info/risk_factors.htm
- Cancer of the Vulva – Cancer Stat Facts [Internet]. SEER. [cited 2019 Aug 13]. Available from: https://seer.cancer.gov/statfacts/html/vulva.html

